Nail biting—or as it’s technically known, onychophagia—can be a frustrating condition for many people to overcome, but one that is not at all uncommon. A better understanding of the causes and issues that come along with chronic nail biting might just make it easier to stop doing it altogether.
Let’s dive into some of the common triggers, treatments and more in a nail biting Q &A.
What are the most common causes of nail biting, both of the casual and chronic varieties?
The exact cause of nail biting is currently unknown, but there are studies that there may be a genetic component. In addition, nail biting may be more common with certain psychiatric disorders such as anxiety and obsessive compulsive disorder (OCD)—though studies are somewhat conflicting on that front. The association of anxiety with onychophagia is controversial with some studies showing no difference in the prevalence of anxiety in nail-biters versus non-nail biters while other studies did report an association. Nail biting has also been shown to be associated with boredom or a lull in activity, which is probably quite relatable to many of us.
How common is nail biting?
Onychophagia is a common disorder affecting 20–30% of the general population. However, its prevalence is likely underestimated as patients are often embarrassed to seek help from physicians
What are the symptoms or recognizable traits of nail biting?
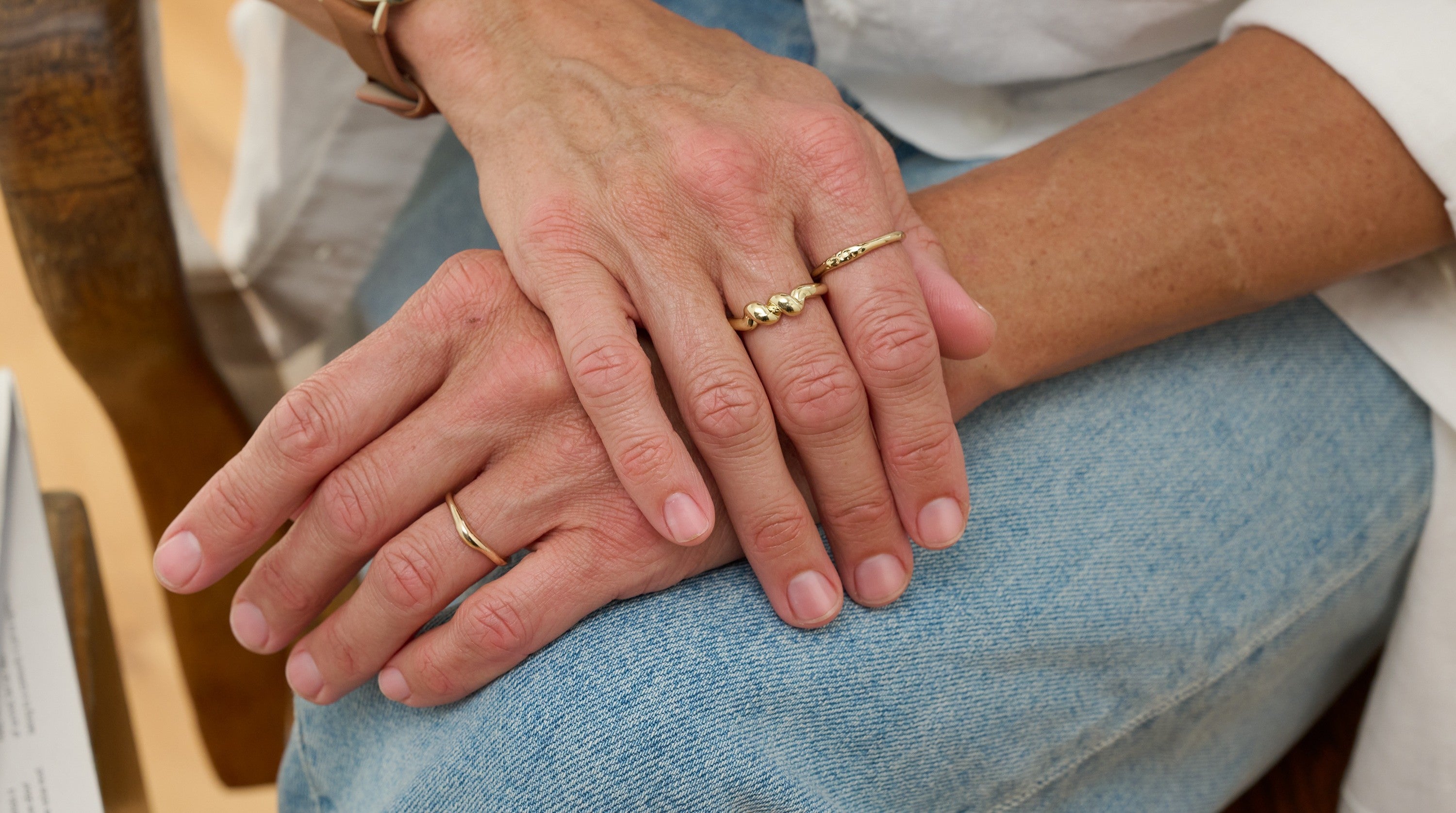
A biter’s nails tend to be abnormally short and uneven. The cuticles may be absent or ragged and nail folds are often in varying stages of healing. Splinter hemorrhages (longitudinal black thin lines in the nail that look like splinters) are often visible. Then there’s the most obvious signal…someone actively biting their nails.
Nail biting can also actually result in nail shape change, creating the development of a shorter, wider nail. Other consequences are white patches aka punctate leuknonychia, which occurs from trauma to the area of the nail where the nail grows from (the matrix – you can see part of it as the lunula or half moon).
Additionally, the oral cavity is a virtual petri dish and can result in the transfer of yeast and bacteria that are normally found in the mouth, but should not be on the nails and fingers and can consequently result in infections of the nail such as paronychias. And, of course, conversely putting your unwashed fingers in your mouth can transfer germs to your mouth, raising the risk of catching a cold or other illness.
What are some other skin, nail, and health issues caused by chronic nail biting
While it may seem simply unattractive, nail biting can actually lead to a host of complications, like:
-
Longitudinal melanonychia: pigmented bands in the nail that can occur from inadvertently stimulating the melanocytes (or melanin-producing cells) that reside in the lunula, or half moon region, of the nail.
-
Paronychia: inflammation of the skin surrounding the cuticle. Paronychias can be chronic (colonized by yeast) or acute (fluctuant, painful, bacterial infections).
-
Herpetic Whitlow: when Herpes virus of the mouth transfers to the finger
-
Oral/dental complications
Are treatment options available for nail biting?
Yes, nail biting is absolutely curable, just like any habit.
Treatments that Dr. Dana recommends include:
-
The habit reversal technique encompasses an awareness of the nail biting activity, warning signs, and the development of a distracting-competing response such as a stress ball, fidget cube or spinner, or rubber band.
-
Bitter nail lacquers that contain unpleasant tasting compounds like denatonium benzoate and sucrose octaacetate can help deter nail biting and are available over the counter.
-
You can use a non-removable reminder like a wristband, as a reminder to stop biting nails.
-
A chronic nail biter may want to explore cognitive behavioral therapy. Discussing habits can be a sensitive subject and one that is best handled by a medical professional.
-
Psychiatric medication may also be a route someone chooses to take under the advisement of a medical professional, perhaps as a way to alleviate some anxiety or symptoms of conditions like the previously mentioned OCD.
-
Try gels or regular manicures to prevent a biter from destroying the nail.
-
There is always the option of physical coverage of the nails with something like gloves or Band-Aids.
Of the treatments Dr. Dana has tried, are there any that show better results?
According to Dr. Dana, her experience with treating onychophagia is that the approach has to be very individualized to the patient and oftentimes she will tweak the regimen as the patient makes progress.
For example, if the cuticles are very damaged and therefore at a higher risk for infection, she will not recommend weekly manicures. If down the road that patient has made clinical progress and the cuticles have healed, she will then consider incorporating salon visits at that point, especially if the patient is someone who does better when the nails are manicured.
Some patients need a physical cover like a glove to get started. What works for one person often does not in another. In general, Dr. Dana likes to discuss a lot of different tactics and give her patients options and to individualize the therapeutic approach based upon the individual. Regular follow-up and collaboration with a cognitive behavioral therapist also often improves outcomes.
She also recommends that her patients keep a diary for several days to get a sense of when they are doing the habit and to see if there is a stimulus like stress or boredom. That way they can initiate habit reversal by having a competing response ready when they are most likely to engage in the habit.